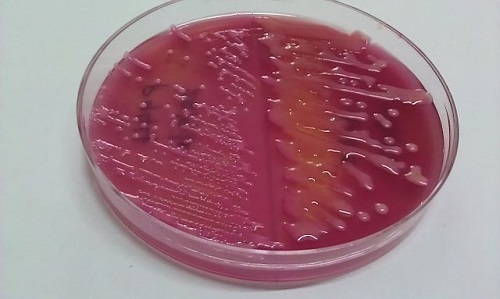
The suspicious guests of your body: Klebsiella Pneumoniae and Escherichia Coli
Getting to know them
When you invite someone to your house you expect them to behave, but in this case we have an opportunist bacteria, K. Pneumoniae, that takes advantage when you are weak. Some genetics variations of this species can cause pyogenic (with pus) liver abscess, antibiotic resistant pneumonia and meningitis (1).
- In the other corner E.Coli, is a commensal (normal flora, a friend) bacteria with some ugly cousins. There is an expectation in the medical community to see an intermediate mutation between members of the Enterobacteriaceae family (bacteria of the gut), like Shigella, and E.Coli, due to the similar genes (2).
When they act the results can be a major hospitalization or more, especially for the more fragile amongst us; elders, toddlers or patients with immune suppression.
K.Pneumoniae is a gram negative (gram stain determines the presence of an external membrane) bacteria that falls in the category of facultative anaerobic, which means it can survive in the presence or absence of oxygen. In the other hand, we have E.Coli, an anaerobic (lives only in the absence of oxygen) gram negative bacteria.
- When do they cause disease?
K.Pneumoniae has different genetic combinations that sometimes can give its impressive defense mechanisms against the immune system (virulence) and make it resistant to multiple and last front antibiotics. For this reason, any compromise to the immune system or misuse of antibiotics, added to an infection with this microbe can lead to a major disease.
E.Coli, on the contrary, produces toxins that require an important immune response, the most dangerous is the toxin called haemolysin, which removes the ferric iron from hemoglobin proteins on the red blood cells, essential to transport oxygen through the bloodstream. This toxin is common in patients with more complicated infections (2).
Due to the abuse and misuse of antibiotics, the resistance to this medication has increased dangerously over the years. The microbiology society published a retrospective article on 2016, analyzing the rise of antibiotic resistance of normal gut flora E.Coli, founding an important increase from 9,4 % in 1980 to 34% in 2010 (3). So, please, do not use antibiotics for a common flu, soared throat or most importantly, without medical prescription.
Symptoms and variations
-
K. Pneumoniae:
In this case, although recent studies show that there are 4 genetically different types of K.Pneumoniae, the methods to identify each one of them are not widespread. So, practically it is divided depending on the symptoms and source of infection:
– Community acquired pneumonia:
It has a quick onset, especially in immune suppression, showing a rapid increase from thick, sometimes bloody mucus to a major infection with pus (abscess formation to empyema), structural damage of the lungs (cavitation) and pleural adhesion…
Interesting fact: the lung is covered by a greasy layer that is actually two fine layers; visceral (attached to the lung) and parietal (external, attached to the ribs, breastbone and spine) pleuras, which usually are separated by 0.2 to 1mililiter of a complex liquid (4), in pleural adhesion, the massive infection of the lungs causes an infection on the pleural liquid, and it turns gluey or fibrotic.
– Urinary tract infection (UTI):
This one can be acquired in the community or in a hospital stay, clinically it is not different from Urinary Infections caused by other bacteria, (burning sensation when urinating, frequent trips to the bathroom, lower back pain) so we would need an analysis of the urine to identify K. Pneumoniae in it.
– Nosocomial (Hospital) Infections:
In this case we have hospitalized patients with invasive procedures like central catheters or mechanic ventilation, others like small children and the immune-suppressed ones that we already know, all with risk factors to be affected by a microbe that as much as we sterilize everything, finds a way to reproduce in hospitals with a constant flow of patients.
There is a variety of hospital infections by K. Pneumoniae: UTI, bloodstream infection (septicemia), infection in open hounds, gallbladder, lungs and bladder catheters. (5)
- Now let’s review the syntomps of infections caused by E. Coli: it has various genetic “brothers” that can get us sick:
- A) Lower urinary infections, septicaemia (general blood infection) or major urinary infections:
In this case the bacteria from the gut, mostly because of poor personal and food hygiene, or some kind of obstruction or retention of urine, ascends through the urinary tract, causing an infection that can go all the way up to the kidneys and even the bloodstream. In children, up to 80% of the brothers of E.Coli can cause Bacterial Meningitis after infecting the bloodstream (2).
- B) Diarrhea.
There are 5 brothers that cause 5 types of diarrhea:
– Entero (gut) Pathogenic (disease inducer) E.Coli: It is common in places with poor social and food hygene, and it causes a mild diarrhea that affects mostly children.
– Entero(gut)toxigenic(produces toxins): Like the name says, this E.Coli produces two kind of toxins that can be deadly to children under 5 years old, or the more vulnerable amongst us. It is also a common diarrhea for travelers whose bodies aren’t used to this bacterium, when traveling to undeveloped countries. (2)
-Enteroinvasive E.Coli: This little enemy has a powerful tool to infiltrate the tissue of the guts: the cells on the walls of the intestines (the good guys) try to eat it, but it can break the little sacs within the cell, breaking the good cop cell and then multiplying in other cells around the neighborhood, causing a mild or moderate bleeding diarrhea. It is mostly transmitted through contaminated food.
-Verotoxigenic E.Coli: Vero cells were used in laboratory cultures to first identify this strains, Vero is an abbreviation in Esperanto of the words “verda reno” and “vero” which means “green kidney” and “truth” respectively, because of the green monkeys of Africa, which has these cells in their kidneys. This E.Coli caused a disruption of these cells, which are really strong cells with unlimited replication. In humans this E.Coli adheres to the cells in the small vessels and causes the destruction of these cells, and it can lead to a Hemorrhagic Colitis or…
The Haemolytic Uraemic Syndrome: This is the most deathly and scary complication of all the strains and infections of E.Coli; the major collapse of the small vessels around the body causes an acute (onset) renal failure, micro-angiopathic hemolityc anemia (decrease of hemoglobin and oxygen flow in the small vessels due to the rupture of red blood cells) and thrombocytopenia (decrease in the number of platelets in the bloodstream –the main cell in cicatrization-) Cattle and raw meat are known to be an important reservoir for the “vero” strain of E.Coli.
– Enteroagregative E.Coli: The last one of the mutant brothers can form a “building” of bacteria, adhering to themselves and the cells of the intestines. It is a cause of chronic diarrhea in undeveloped countries but rare in the industrialized ones.
Most of the strains (including the normal flora in the gust) can acquire different manifestations depending on the location, power of the strain for infection, and vulnerability of the patient. (2)
Prevention before treatment
- Pneumoniae multiplies easily in dense water with lots of minerals such as industrial wastes and wash taps (6). In the hospital environment, the sneezing and coughing of other patients is another way of propagation.
Prevention therefore, would be directed to clean water solutions from politicians and at home, as well as the proper sterilization in hospitals and the use of medical mask for patients with K. Pneumoniae infections.
The treatment of complicated, antibiotic resistant infections by this microbe, require extensive lab test and a possible combination of antibiotic, as approved by the FDA in 2015 (7).
-
E.Coli
Contaminated food and water are the main vehicles of infection, especially in developing countries, so again the changes must be in the social and political sphere within these regions.
Travelers of industrialized countries going to places with poor food and water hygiene should consume only bottled water, and fresh cooked meals. In this case it is not transmitted through the air, since this is an anaerobic bacterium, like we learned at the beginning.
In hospitals the infection is usually hand to hand, so the sanitary measures of all the hospital staff should be according to the highest standards, as possible.
Treatment of colitis by E.Coli, mostly in form of diarrhea, consist of an early and thorough hydration and antibiotic use is really NOT recommended without the proper feces analysis, to confirm if there actually is a dangerous microbe causing the disease.
That was it, simpler than it looks, now let’s review the major differences between these 2 microbes:
| Item | K. Pneumoniae | E.Coli |
| Classification | Gram (-) Facultative anaerobic | Gram (-) Just Anaerobic
|
| Opportunist bacteria | Normal “gut” bacteria | |
| When do they cause serious disease? | Depending on the virulence of the Strain | If there is a major toxin production |
| Symptoms and diseases that they cause | Pneumonia, empyema, pleural adhesion, UTI, infections on open hounds, gallbladder and bladder catheters. | UTI, diarrhea, bleeding diarrhea, bloodstream infection, meningitis, Haemolytic Uremic Syndrome |
| Prevention | Water and food cleansing and medical masks on hospitals | Water and food cleansing and well, but on hospital washing hands |
| Treatment | May require multiple lab test and therapy with two or more antibiotics depending on drug resistance of the strain. | Only hydration and antibiotics after the feces analysis. |









Leave a Reply