
What is Arthritis?
Arthritis is referred to as any disorder that affects the joints through joint inflammation.
It causes stiffness, swelling, and pain in the joints which makes it painful to move around.
Joints are places in the body where the two bones meet.
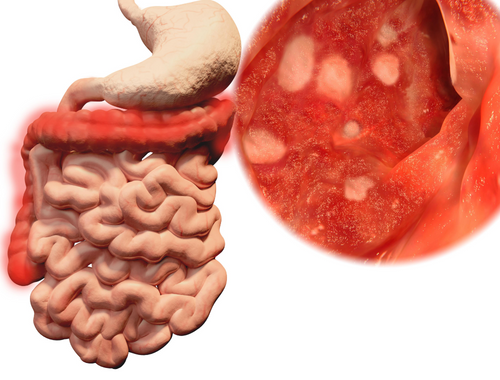
What is Ulcerative colitis (UC)?
Ulcerative colitis is one of the two types of inflammatory bowel disease (IBD).
It is referred to as a long-term condition where the rectum and the colon stay inflamed.
The colon is the longest part of the large intestine, and the rectum is the ending area of the large intestine where the stool is stored.
UC can also cause Ulcers in the digestive tract.
Some of the complications of Ulcerative Colitis include fever, abdominal cramping, severe rectal bleeding, severe dehydration, rapidly swelling colon, and weight loss.
UC has no known cure and aggravated symptoms can result in life-threatening conditions.
However, appropriate treatment can alleviate symptoms of UC and result in long-term remission of the disease.
What is the relationship between Ulcerative colitis (UC) and Arthritis?
Although UC mainly affects the large intestine, it is deduced that it affects other body parts as well.
The most common influence on patients with UC is arthritis, however, it is not easy to determine if arthritis in a patient is due to UC.
Unlike rheumatoid arthritis, arthritis that is due to Ulcerative Colitis is not that severe. The joints do not usually go through destructive changes and joint involvement is unsymmetric.
Except for one form of arthritis which is Ankylosing spondylitis (discussed later), it is concluded through the studies that the arthritis symptoms subside if the patients get appropriate treatment for UC.
Arthritis associated with Ulcerative Colitis is categorized into three categories:
- Peripheral arthritis
- Axial spondyloarthritis (axSpA)
- Ankylosing spondylitis
Out of the above-mentioned arthritis, Peripheral Arthritis is the one that is mostly found in UC patients with a 19.6% assurance rate.
It is also observed that patients of UC have a different experience of arthritis pain compared with those who do not have UC.
Patients with UC develop arthritis at a younger age but most do not have joint damage that is long-term or lifelong.
Peripheral arthritis
Peripheral arthritis affects arms, legs, elbows, wrists, knees, and ankles. The pain usually moves from one joint to the other.
As stated above it is the most common form of joint pain that occurs in UC patients.
The level of joint inflammation generally corresponds with the extent the colon is inflamed.
The symptoms of peripheral arthritis mostly subside and even disappear as the UC symptoms get controlled.
Axial spondyloarthritis (axSpA)
This form of arthritis causes pain in the sacroiliac joints and the lower spine.
The joint pain through Spondylitis appears months or sometimes even years before the patient experiences any UC symptoms.
This type of arthritis can result in the fusion of parts of the spine, leading to the reduction of a person’s range of motion.
Ankylosing spondylitis
Ankylosing spondylitis is a rare complication of UC. It causes inflammation in sacroiliac joints and the spine but can affect the heart valves, eyes, and lungs. It is a severe form of Axial spondyloarthritis.
If a person has Ankylosing spondylitis, it can cause long-term damage and the patient may require getting the colon removed surgically.
This type of arthritis affects the patient’s flexibility by making the back stiff and forcing the patient into a permanently distorted posture.
The effects of this type of arthritis don’t subside or reverse if the patient receives treatment for UC.
People with genetically occurring Urinary tract infection and a predisposition to bowel tends to develop Ankylosing spondylitis.
This usually appears in the early 30 years of life.
How to treat arthritis in patients with UC
A rheumatologist can most efficiently diagnose arthritis in UC patients.
Arthritis patients, who do not have UC, are usually prescribed nonsteroidal anti-inflammatory drugs, such as ibuprofen or aspirin.
However, if this patient has UC symptoms as well, these medications are not recommended since they can further irritate the intestine.
In such a case, the doctor might prescribe a biological drug that calms the immune system since these medicines treat UC as well as Arthritis.
Since UC patients are more prone to develop arthritis, therefore, it is recommended to reduce their risk of arthritis by eating a healthy and anti-inflammatory diet, lowering stress levels, and avoiding certain foods such as dairy products and fiber-rich products.
Summary
- Ulcerative Colitis is the inflammation of the rectum and the colon.
- Arthritis is referred to as any disorder that affects the joints through joint inflammation.
- Ulcerative Colitis can affect other body parts apart from the large intestine.
- One of the most common influences on patients with UC is arthritis.
- Arthritis associated with UC is categorized into three categories: Peripheral arthritis, Axial spondyloarthritis (axSpA), and Ankylosing spondylitis.
- Peripheral Arthritis is mostly found in UC patients with a 19.6% assurance rate.
- Peripheral Arthritis symptoms subside if the patients get appropriate treatment for UC.
- Ankylosing spondylitis, although occurs rarely in UC patients but causes permanent and severe effects.
- A rheumatologist can most efficiently diagnose arthritis in UC patients.
- Patients of arthritis who have UC are not prescribed nonsteroidal anti-inflammatory drugs, since they can further irritate the intestine.
- In such a case, a biological drug that calms the immune system is effective since these medicines treat UC as well as Arthritis.
- UC patients can reduce their risk of developing arthritis by taking an anti-inflammatory diet, avoiding dairy products, and lowering stress levels.
FAQs:
What are 3 common complications of someone with ulcerative colitis?
Three common complications, that a person with ulcerative colitis can face, are Severe bleeding, Severe dehydration, and rapidly swelling colon, also called toxic megacolon.
What other autoimmune diseases are common with ulcerative colitis?
Osteoporosis, Bowel Cancer, Primary sclerosing cholangitis (PSC), Fibromyalgia, Ulcer, and Diabetes are some autoimmune diseases that are common with ulcerative colitis.
Can a rheumatologist help with ulcerative colitis?
A gastroenterologist is a doctor who treats digestive disorders including Ulcerative colitis whereas a Rheumatologists specialize in treating autoimmune disorders and related health problems.
However, due to the findings that Ulcerative colitis is an autoimmune disorder and given the systemic manifestations of IBD, it is very much likely that a rheumatologist can help patients with ulcerative colitis and Crohn’s disease.
Does colitis cause arthritis?
The findings of the Crohn’s and Colitis Foundation confirm that those people who have Ulcerative colitis tend to have one of the three forms of arthritis and when Ulcerative colitis is controlled after the appropriate treatment, the joint pain and symptoms typically improve.
Can ulcerative colitis cause rheumatoid arthritis?
Multiple studies conclude that a number of patients with Ulcerative colitis (UC) develop Rheumatoid Arthritis (RA) within a few years hence there is a relationship between UC and RA.
What helps arthritis pain with ulcerative colitis?
Treating Arthritis by taking pain relievers like ibuprofen or aspirin often irritates the stomach lining if taken for a long time. This is the reason doctors usually prescribe drugs to treat Ulcerative colitis and after finishing this treatment the joint pain usually subsides.
These drugs include prednisone or sulfasalazine.
The doctor might also prescribe a biological drug that calms the immune system since these medicines treat UC as well as Arthritis.
What are the red flags for ulcerative colitis?
The most common warning signs of Ulcerative Colitis are excruciating abdominal pain and bloody diarrhea.
Which drug is used in ulcerative colitis and rheumatoid arthritis?
Sulfasalazine is a drug that belongs to the medicinal group of amino salicylates and is used to treat ulcerative colitis as well as rheumatoid arthritis
How often do I need a colonoscopy with ulcerative colitis?
Regular colonoscopies are recommended for people with UC as they have an increased risk of colorectal cancer. It is recommended, for the person who has had UC symptoms for the past 8 years, to get a colonoscopy done every 1-2 years.
When is ulcerative colitis an emergency?
UC can be life-threatening if a person experiences worsening symptoms such as severe stomach pain, high fever, bloody diarrhea, rapid heart rate, and heavy rectal bleeding.
This situation is called Acute severe ulcerative colitis (ASUC) which is a serious complication of Ulcerative colitis.
ASUC is a medical emergency, and the person needs to be hospitalized to get the proper treatment.
Is ulcerative colitis a disability?
Ulcerative colitis is a disability if it has severe symptoms that affect a person’s workability and quality of life. Some people who have UC are also provided disability benefits, in a few countries, including Medicare and parking permits.












Leave a Reply