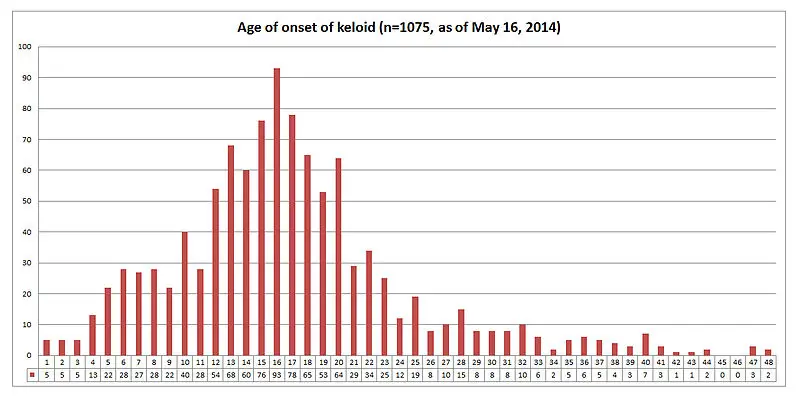
Why do keloids form?
A keloid is an abnormal proliferation of scar tissue that develops at the site of skin injury e.g. on the site of a surgical incision or trauma. It does not regress and grows beyond the actual margins of the wound. Keloids should not be confused with hypertrophic scars, which are merely elevated scars that do not grow beyond the boundaries of the original wound and may reduce over time.
Anyone, at any age can develop a keloid. Studies have shown that there are some skin types and ages who are more prone to keloids. It has been found that there is a higher occurance of keloids between the ages of 10 and 30 years age, with the average age of keloid sufferers being in their early 20’s; they are not so common in extremes of age. It is equally common in men and women, although women in general may have more keloids due to a higher incidence of piercings. It has also been found that certain skin types are also more susceptible to keloid formation. The frequency of keloid occurrence in persons with highly pigmented skin is 15 times higher than in persons with less pigmented skin. Family history is also important and currently evidence is pointing to there being a genetic cause involved in keloid formation, and if a family member has them you are more likely to develop a keloid on a wound and even more so if a twin has developed keloids.
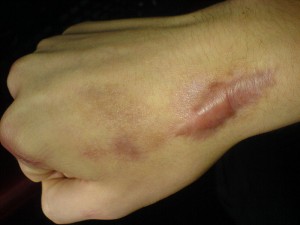 Keloids are fibrotic lesions of the skin where dead fibrous tissue has formed, that is a variation of the normal wound healing process. During the normal process of healing, there is a balance between the production and the breakdown of collagen, which is a protein that makes up the fibres of the skin. With keloidal scars, the cells in the skin called fibroblasts produce excessive amounts of collagen. The collagen fibrils in keloids are more irregular, abnormally thick, and have unidirectional fibers arranged in a highly stressed orientation. This leads to a thick, raised appearance that is characteristic of the keloidal scars.
Keloids are fibrotic lesions of the skin where dead fibrous tissue has formed, that is a variation of the normal wound healing process. During the normal process of healing, there is a balance between the production and the breakdown of collagen, which is a protein that makes up the fibres of the skin. With keloidal scars, the cells in the skin called fibroblasts produce excessive amounts of collagen. The collagen fibrils in keloids are more irregular, abnormally thick, and have unidirectional fibers arranged in a highly stressed orientation. This leads to a thick, raised appearance that is characteristic of the keloidal scars.
A relationship appears to exist between immunoglobulins and keloid formation; while levels of immunoglobulin G and immunoglobulin M are normal in the serum of patients with keloids, the concentration of immunoglobulin G in the scar tissue is elevated when compared to hypertrophic and normal scar tissue. Keloids usually occur during the healing of a deep skin wound. Keloid formation can occur within a year after injury, and keloids enlarge well beyond the original scar margin.
The most frequently involved sites of keloids are areas of the body that are constantly subjected to high skin tension. Wounds on the chest, shoulders, flexor surfaces of the extremities (eg, deltoid region), and throat region and wounds that cross skin tension lines are more susceptible to abnormal scar formation. Rarely, spontaneous keloids occur without a history of trauma.
Summary:
Unfortunately, the fact that medical science does not know the exact reasons why keloids form in some people and not in others, means that the best way to deal with a keloid is not to get one in the first place. In other words, a person who already has a keloid should choose not to have elective surgery, or get their ears pierced, or pursue body piercing and avoid trauma/injuries. Prevention is necessary because treatment is not always completely successful, or may not work at all.








Leave a Reply